- Jeffrey Peng MD
- Mar 4
- 5 min read
By Dr. Jeffrey Peng, MD · Published March 4, 2026 · 6 min read
Watch the Full Video
A Baker's cyst — also called a popliteal cyst — is a fluid-filled swelling that develops in the back of the knee. Named after the British surgeon Dr. William Baker, who first described the condition, it can range from a painless incidental finding on an MRI to a significant source of discomfort that limits everyday activities like bending, squatting, and walking.
In my practice, Baker's cysts are one of the most common reasons patients come in with posterior knee pain. Understanding what causes the cyst, how it is treated, and what you can do to prevent recurrence is essential for long-term management.
What Is a Baker's Cyst?
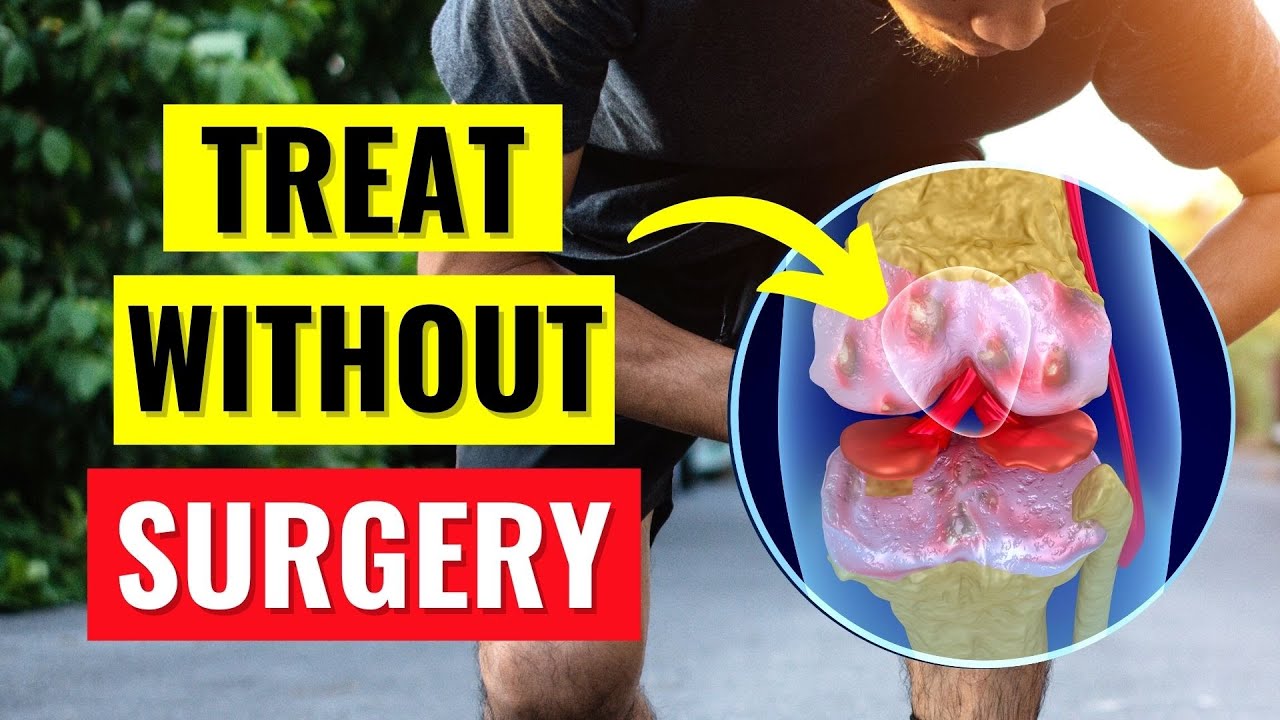
A Baker's cyst forms when excess fluid accumulates in the popliteal fossa, the soft tissue space behind the knee joint. The knee naturally produces synovial fluid to lubricate the joint, but when something inside the knee causes irritation or inflammation, the body produces more fluid than usual. That extra fluid can migrate toward the back of the knee and collect in a pouch, forming the cyst.
Symptoms vary from person to person. Some patients notice a visible lump or swelling behind the knee. Others describe a sensation of tightness or fullness, especially when bending the knee fully. However, many Baker's cysts are completely asymptomatic and are discovered incidentally during imaging for an unrelated issue.
What Causes a Baker's Cyst?
A Baker's cyst almost always develops as a secondary problem — meaning there is an underlying condition inside the knee that is driving excess fluid production. The cyst itself is the symptom, not the root cause.
The most common underlying cause is osteoarthritis of the knee. The grinding, catching, and cartilage wear associated with arthritis triggers chronic inflammation and fluid buildup. Over time, that fluid flows posteriorly and forms the cyst.
Meniscus tears — particularly tears of the posterior horn — are the second most common contributor. A torn meniscus disrupts normal knee mechanics, leading to irritation, inflammation, and increased synovial fluid production.
One important detail: the flow of fluid into the popliteal fossa is essentially a one-way street. Once fluid collects behind the knee, it is difficult for the body to reabsorb it on its own. This is why Baker's cysts tend to persist or enlarge if the underlying cause is not addressed.
How Is a Baker's Cyst Diagnosed?
A thorough physical examination is the first step. Your physician will assess the back of the knee for swelling, tenderness, and range of motion. If a Baker's cyst is suspected, ultrasound is the quickest and most cost-effective way to confirm the diagnosis. The key anatomical landmarks are the semimembranosus tendon and the medial head of the gastrocnemius muscle, which border the cyst.
An MRI may also reveal a Baker's cyst, and in many cases, it provides additional information about the underlying cause — such as cartilage damage or a meniscus tear — that prompted the cyst to form in the first place.
Not All Posterior Knee Pain Is a Baker's Cyst
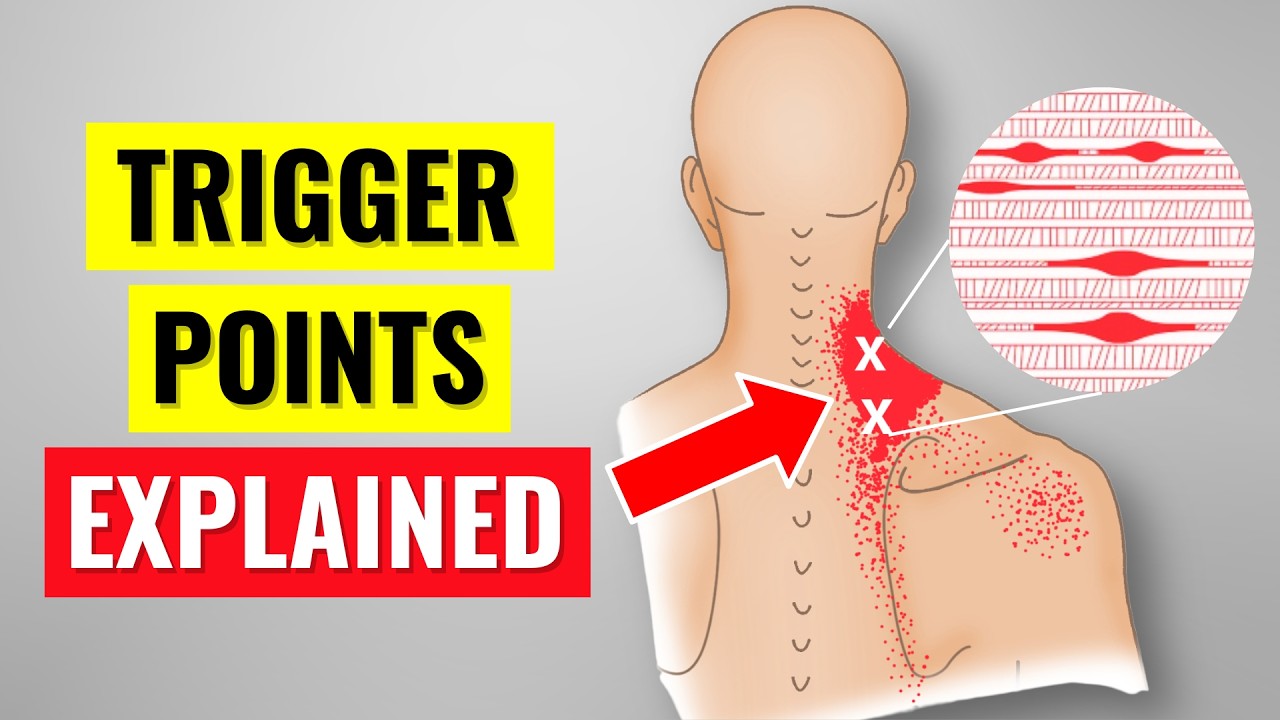
It is worth noting that posterior knee pain has several possible causes beyond a Baker's cyst, especially when there is no visible swelling. Other diagnoses to consider include tendinopathy of the popliteus tendon and myofascial trigger points within the medial and lateral heads of the gastrocnemius muscle. Trigger points in the muscles surrounding the knee are commonly overlooked as a source of pain and can significantly contribute to both discomfort and functional limitations.
What Are the Treatment Options for a Baker's Cyst?
Treatment depends on the size of the cyst and the severity of symptoms.
Small or Asymptomatic Cysts
Small Baker's cysts that cause no symptoms generally do not require treatment. These are often discovered incidentally on imaging and can be safely monitored over time.
Mild Symptoms
For patients with mild discomfort, several conservative measures can help. Applying ice to the back of the knee reduces swelling and pain. A compression bandage or neoprene knee brace can provide support and limit fluid accumulation. Over-the-counter anti-inflammatory medications such as ibuprofen or naproxen may also be beneficial. Physical therapy and targeted rehabilitation exercises play an important role in symptom management and recurrence prevention.
Larger, Symptomatic Cysts
Larger Baker's cysts that cause significant discomfort or interfere with activity often require more direct intervention. Ultrasound-guided aspiration is a fast, safe, and effective in-office procedure. During this procedure, a physician uses ultrasound imaging to drain the fluid from the cyst and then injects medication — typically a corticosteroid — to help close the cyst wall and reduce inflammation.
In my practice, I often combine cyst aspiration with an intra-articular knee injection to address the inflammation inside the joint itself. By treating both the cyst and the underlying source of excess fluid production, we achieve better long-term outcomes. Because ultrasound-guided therapies are so effective, surgical intervention for a Baker's cyst is rarely necessary.
What Happens If a Baker's Cyst Ruptures?
One potential complication of a Baker's cyst is rupture. Excessive pressure within the cyst can cause it to burst, releasing fluid into the calf. This typically results in sudden, sharp pain and swelling that extends from the back of the knee down into the lower leg. The symptoms can mimic a deep vein thrombosis (DVT), which is why prompt evaluation is important to rule out a blood clot and confirm the diagnosis.
If a cyst rupture is confirmed, aspiration of the remaining fluid and supportive care — including ice, compression, and elevation — usually provide effective symptom control.
How Do You Prevent a Baker's Cyst From Coming Back?
The single most important step in preventing a Baker's cyst from recurring is treating the underlying cause. If osteoarthritis is driving the excess fluid, managing the arthritis through weight management, physical therapy, activity modification, and appropriate joint injections (such as PRP or hyaluronic acid) will reduce the likelihood of cyst recurrence.
If a meniscus tear is the culprit, addressing the tear — whether through conservative rehabilitation or, in select cases, surgical repair — is essential. Without treating the root problem, draining the cyst alone will only provide temporary relief, and the cyst will likely return.
If you are dealing with a Baker's cyst or persistent posterior knee pain, schedule a consultation to discuss your options and develop a personalized treatment plan.
Medical Disclaimer: This content is for educational purposes only and does not substitute for the medical advice of a physician. Always consult your healthcare provider before beginning any new treatment program. The information presented reflects the opinion of Dr. Jeffrey Peng and does not represent the views of his employers or affiliated hospital systems.